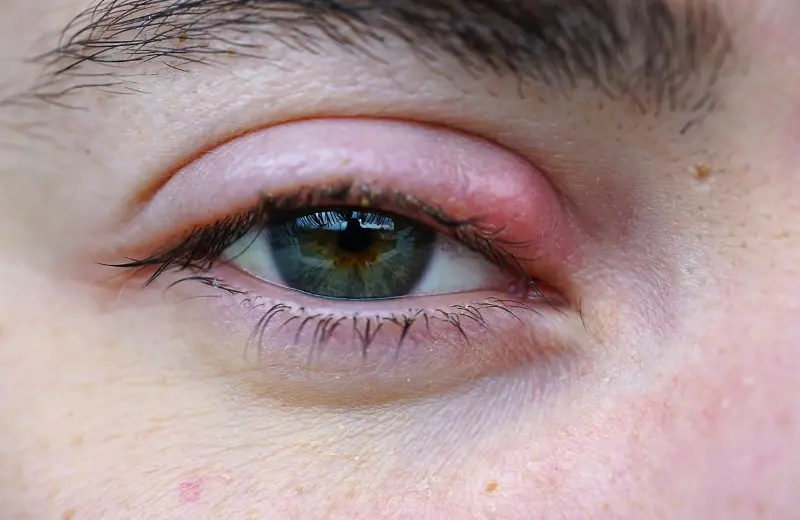
A stye has a way of making itself known fast. One morning your eyelid feels a little tender, and by the next day, there’s a red, swollen lump that makes blinking uncomfortable. Catching a stye in its beginning stages of eye stye development gives you the best chance to treat it at home and stop it from progressing into a more painful, larger infection.
In these initial phases, a stye appears as a small, tender, red bump on the edge of the eyelid—either on the outer rim (external) or under the eyelid (internal). The early signs include localized eyelid pain or tenderness, mild swelling, a persistent sensation of having something in your eye, and slight redness concentrated around the lash line.
What Is a Stye?
A stye (medical name: hordeolum) is a bacterial infection of the elands in the eyelid. There are two types:
| Type | Location | Cause |
|---|---|---|
| External stye (most common) | On the eyelid edge, at the base of a lash | Infection of the eyelash follicle or glands of Zeis |
| Internal stye | Inside the eyelid (less visible, more painful) | Infection of the meibomian gland |
Both are most often caused by *Staphylococcus aureus* bacteria – the same bacteria responsible for many skin infections.
Early Stage Symptoms – Day 1 to Day 2
In the beginning, a stye is easy to miss or dismiss as irritation:
- Eyelid soreness or tenderness – usually localized to one spot on the upper or lower lid
- Redness at the eyelid margin – a faint pink or red area near the lash line
- Mild swelling – the eyelid may feel slightly puffy in one area
- Sensation of a foreign body – feeling like something is in the eye
- Sensitivity to light – mild photophobia
- Watery eyes – the eye may respond to irritation with excess tearing
At this stage, there may be no visible bump yet – just tenderness and slight redness.
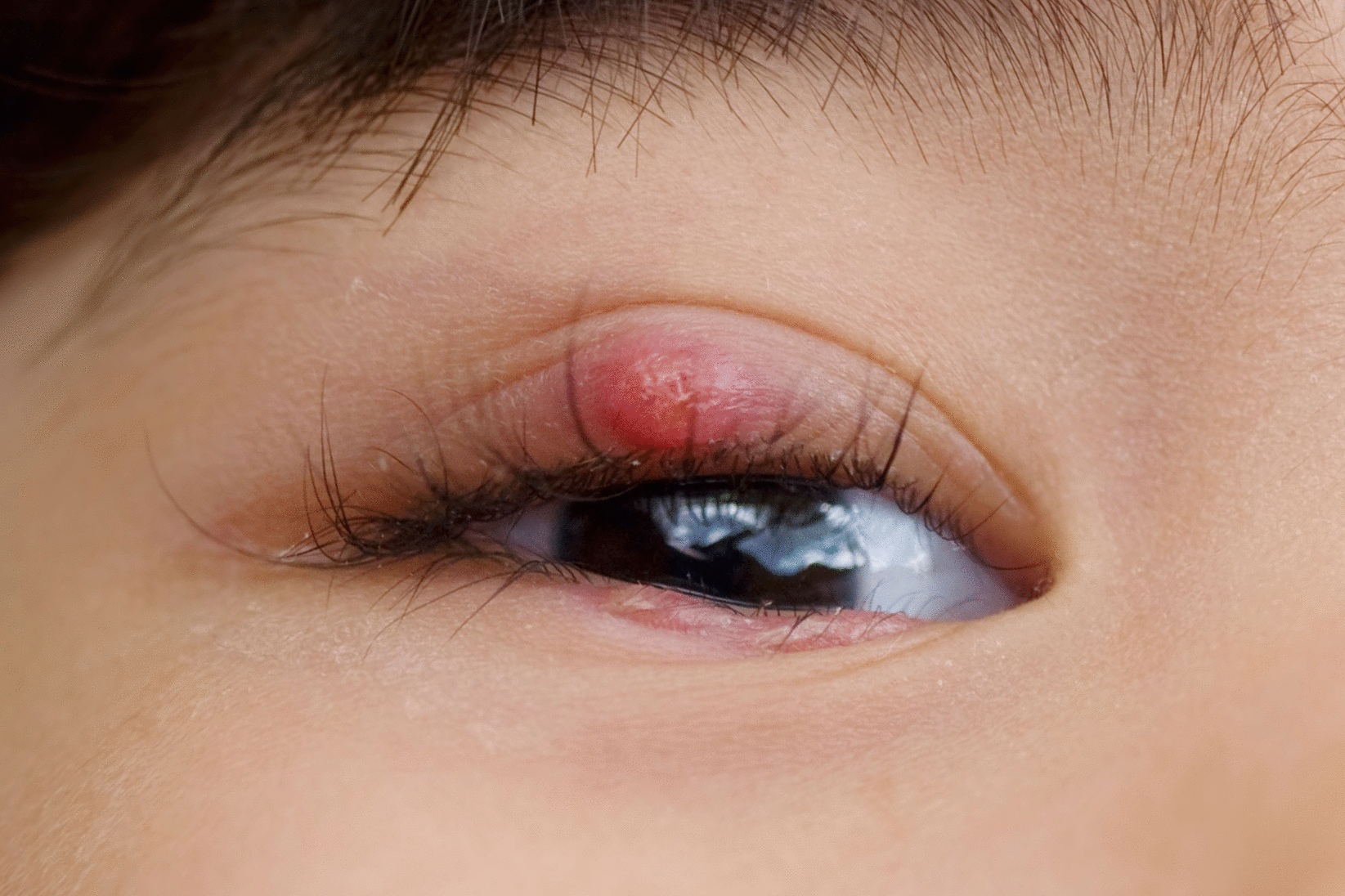
Day 2 to Day 3 – The Bump Appears
Within 24-48 hours of the first symptoms, a small, round bump becomes visible:
- Located on the eyelid edge, often at the base of an eyelash
- Red and warm to the touch
- Tender when pressed
- May be topped with a tiny yellow or white spot (a pus head forming)
This is still early enough for effective home treatment.
What Causes Styes to Form?
| Contributing Factor | Why It Matters |
|---|---|
| Touching eyes with unwashed hands | Transfers Staph bacteria |
| Sleeping in eye makeup | Blocks and irritates glands |
| Old or shared cosmetics | Contaminated with bacteria |
| Chronic blepharitis | Inflammation of eyelid margins increases vulnerability |
| Stress and immune suppression | Lowers resistance to bacterial infection |
| Contact lens handling without handwashing | Direct bacterial transfer |
| Previous styes | Creates scar tissue; increases recurrence risk |
What to Do in the Early Stages
The earlier you start treatment, the faster it resolves – and the less likely it is to need medical intervention.
Warm Compress – The Most Important Step
Heat is the primary treatment for styes. It:
- Increases blood flow to the area, speeding immune response
- Helps soften and liquefy the blocked secretion so it can drain naturally
- Reduces pain and swelling
How to do it:
- Soak a clean cloth in warm (not hot) water and wring it out
- Hold against the closed eyelid for 10-15 minutes
- Repeat 3-4 times per day
- Use a clean cloth each time to avoid reinfection
Purpose-made heated eye masks (like Bruder masks) maintain heat longer and are worth investing in for recurrent styes.
Do not squeeze or pop the stye. Squeezing spreads bacteria and can push the infection deeper or into the bloodstream in rare cases.
Keep the Area Clean
- Wash hands thoroughly before touching your face or eyes
- Remove all eye makeup until the stye resolves
- Gently clean the eyelid margin with diluted baby shampoo or a dedicated eyelid wipe
- Don’t wear contact lenses while you have a stye
Don’t Share Eye Products
Mascara, eyeliner, and eye shadows should not be shared – and if you have a stye, replace your current eye makeup afterward to avoid reinfection.
What NOT to Do
- Don’t pop or squeeze it – this spreads infection
- Don’t wear contact lenses – increases irritation and infection risk
- Don’t use “get the red out” eye drops – these do nothing for a stye and may irritate further
- Don’t use someone else’s eye drops – risk of cross-contamination
Timeline of a Typical Stye
| Day | What to Expect |
|---|---|
| Day 1-2 | Tenderness and redness without visible lump |
| Day 2-4 | Visible bump appears; pus may begin to form |
| Day 4-7 | Stye comes to a head; may drain on its own |
| Day 7-14 | Resolves completely with proper care |
Most styes, treated with warm compresses, resolve within 7-10 days.
Chalazion vs. Stye – Know the Difference
A chalazion is often confused with a stye:
| Feature | Stye | Chalazion |
|---|---|---|
| Pain | Yes – tender | Usually painless |
| Cause | Bacterial infection | Blocked meibomian gland (no infection) |
| Location | At eyelid edge, near lash | Further from eyelid margin |
| Onset | Rapid (days) | Gradual (weeks) |
| Treatment | Warm compress, antibiotics if needed | Warm compress; may need drainage |
When to See a Doctor
Most styes resolve on their own. See a doctor if:
- The stye doesn’t improve after 1-2 weeks of warm compress treatment
- The entire eyelid becomes swollen
- Redness and swelling spread to the cheek or surrounding skin
- Vision is affected
- The stye is very large and painful
- You have recurrent styes (may need longer antibiotic treatment or investigation of underlying skin conditions like rosacea or seborrhea)
A doctor may prescribe antibiotic ointment or eye drops. Rarely, a stye may need to be lanced and drained under local anesthetic.
Bottom Line
A stye is easiest to treat in its earliest stage – when you notice tenderness or a small red spot before a full bump forms. Start warm compresses immediately, keep the area clean, and resist the urge to pop it. Most styes resolve completely within 1-2 weeks with consistent home care. If it persists or spreads, a quick doctor’s visit can prevent a minor issue from becoming a bigger one.